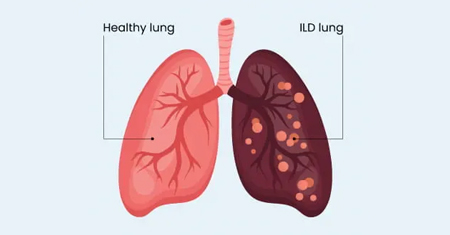
Interstitial Lung Disease (ILD)
Interstitial Lung Disease (ILD) represents a group of complex lung disorders characterized by inflammation and scarring of the lung tissue, leading to progressive breathlessness and reduced oxygen exchange.
Under the specialized care of Dr. Amolkumar Achlerkar, ILD is managed through precise diagnostic evaluation, advanced imaging, and evidence-based therapeutic strategies focused on slowing disease progression and preserving lung function.
Understanding Interstitial Lung Disease
ILD affects the interstitium — the delicate tissue surrounding the lung air sacs. Over time, inflammation may lead to fibrosis (scarring), causing stiffness of the lungs and difficulty in oxygen transfer to the bloodstream.
Early identification is critical, as certain forms of ILD can progress rapidly without structured medical intervention.
Common Causes & Risk Factors
- Autoimmune or connective tissue disorders
- Long-term occupational exposure to dust or chemicals
- Smoking history
- Certain medications
- Post-infectious or post-COVID lung injury
- Idiopathic (unknown cause)
Typical Symptoms
- Progressive breathlessness
- Persistent dry cough
- Fatigue and reduced exercise capacity
- Unexplained weight loss (in advanced cases)
- Low oxygen levels
Advanced Diagnostic Evaluation
Accurate diagnosis and staging of ILD require a comprehensive evaluation that may include:
- High-Resolution CT (HRCT) scan of the chest
- Pulmonary Function Testing (PFT)
- 6-Minute Walk Test (6MWT)
- Autoimmune and blood profile testing
- Bronchoscopy or lung biopsy (when indicated)
This multi-dimensional approach ensures precise diagnosis and tailored treatment planning.
Comprehensive Treatment Approach
Treatment strategies are individualized based on the type and severity of ILD. Management may include:
- Anti-fibrotic medications
- Immunosuppressive therapy (where indicated)
- Oxygen therapy for advanced cases
- Pulmonary rehabilitation programs
- Regular lung function monitoring
The primary goal is to slow progression, relieve symptoms, and maintain optimal respiratory performance.
When to Consult a Specialist
- Unexplained progressive breathlessness
- Persistent dry cough without clear cause
- Abnormal HRCT findings
- Low oxygen saturation levels
- Family history of pulmonary fibrosis
Early specialist consultation significantly improves long-term outcomes and helps prevent irreversible lung damage.